COVID-19 Management: Co-morbidities and Co-infection

How do co-morbidities and co-infection with other infectious diseases affect our management of COVID-19?
Here we highlight key conditions that clinicians should be aware of.
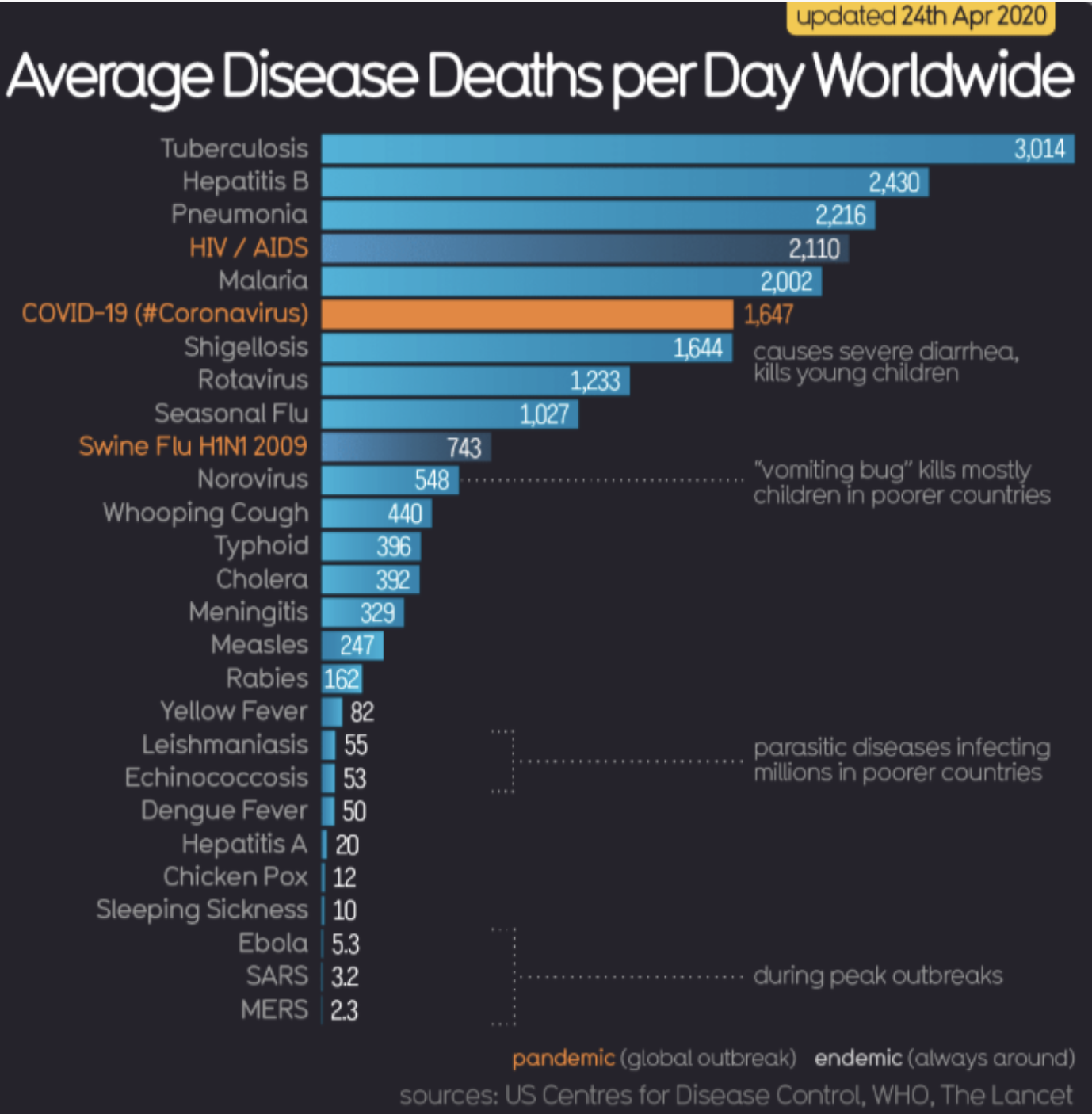
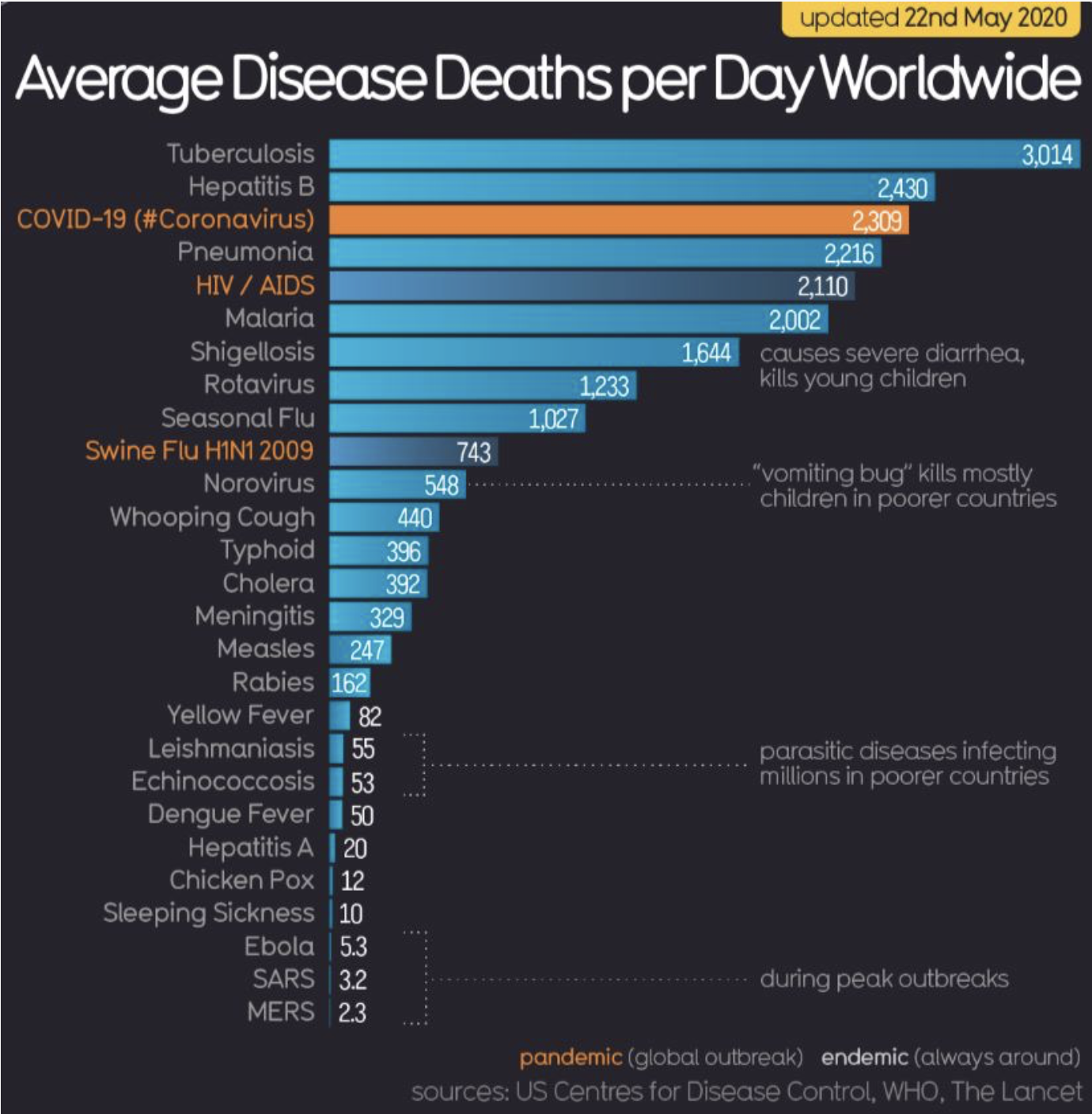
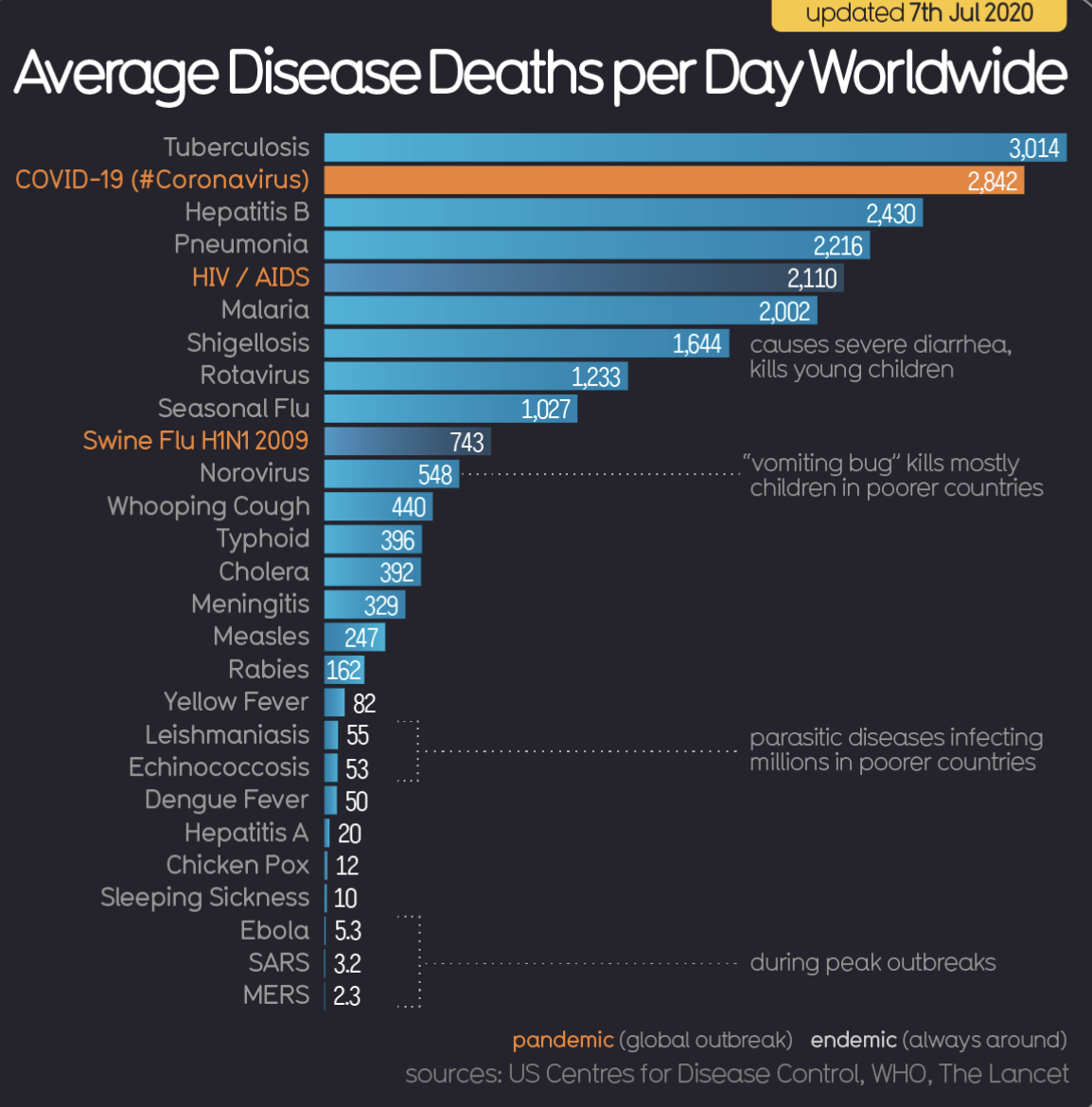
Average Disease Deaths per Day Worldwide:
Compare the graphs from April to June 2020; in roughly two months, COVID-19 has over taken pneumonia, malaria and HIV/AIDS as a cause of death worldwide.
Image Source: Information is Beautiful
HIV and COVID-19
"At present there is no evidence that the risk of infection or complications of COVID-19 is different among people living with HIV who are clinically and immunologically stable on antiretroviral treatment when compared with the general population. "
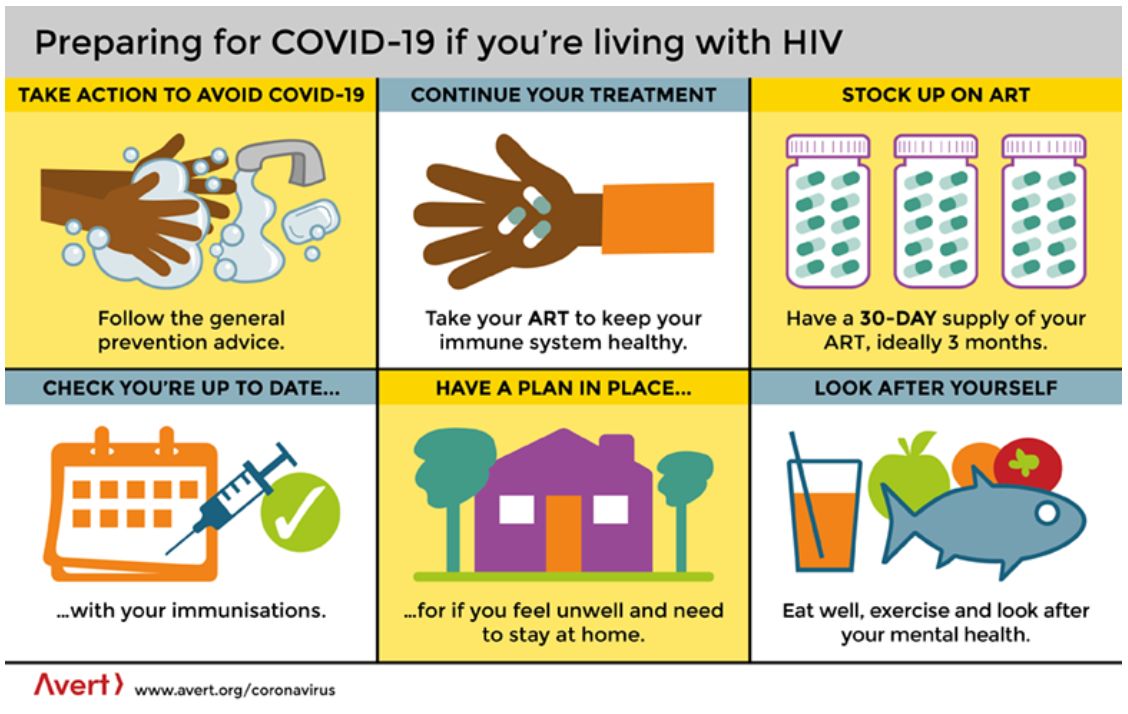
Medication for treatment of HIV (lopinavir and darunavir boosted by ritonavir or cobicistat) have not been shown to be effectiveve treatments for COVID-19 are not efficacious against severe acute respiratory syndrome coronavirus [1, 2, 3]
Therefore the WHO does not recommend the changing of antiretroviral combinations in an attempt to treat COVID-19 in HIV patients [1].
Data on HIV and COVID-19 is still emerging.
For more examples, view this case series of 5 patients from Spain, Barcelona, published in the Lancet.
Tuberculosis (TB) and COVID-19:
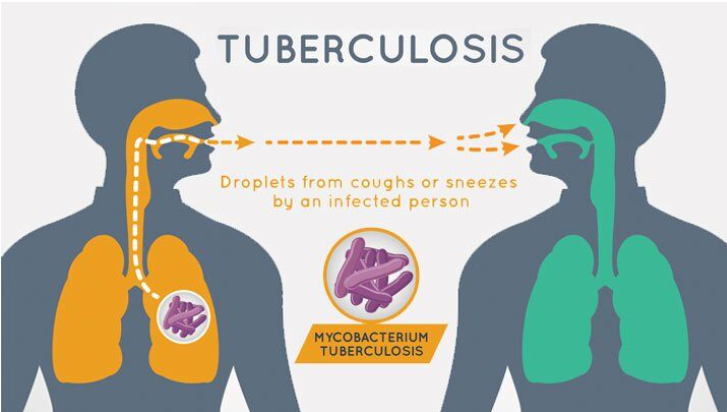
WHO Webinar on TB in the COVID-19 pandemic
Summary:
TB treatment is the same for patients with or without COVID-19 infection
Currently there is no evidence that the BCG vaccine can be used for routine COVID-19 prophylaxis
BCG for at-risk newborns should still be undertaken
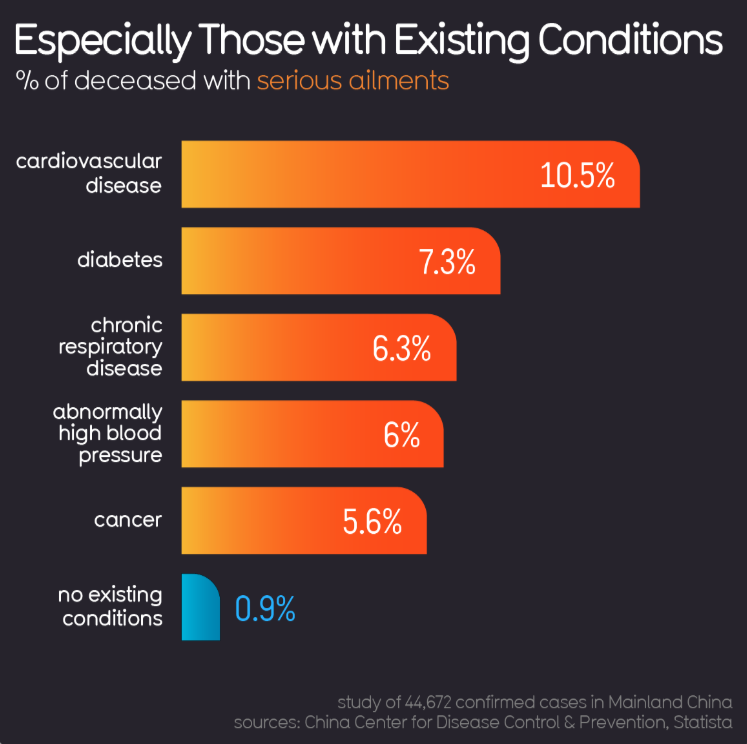
Co-Morbidities and COVID-19
“COVID-19 can negatively impact NCD outcomes for adults and children through several pathways including the higher susceptibility to COVID-19 infection and higher case fatality rates among people with NCDs; delays in diagnosis of NCDs resulting in more advanced disease stages; delayed, incomplete or interrupted therapy (treatment, rehabilitation, palliation) of NCDs”
- WHO, Maintaining essential health services: operational guidance for the COVID-19 context
Is shielding good?
In the UK, individuals who had certain comorbidities were considered higher-risk for developing complications and have a poor outcome if they caught COVID-19. Therefore advised to self-isolate at home for 12 weeks at the start of the pandemic – the “Shielded” group. Advice from UK specialist organisations and GP practices also helped generate criteria and assess patients on a case-by-case basis [4]. As of 20 May 2020, over 2 million individuals, 3.97% of the UK population were identified to be in the “Shielded” group.
This video by the Centers for Disease Control and Prevention (CDC), USA summarises advice and individuals who are at Higher Risk for Severe Illness.
As more data and research emerge on co-infection and co-morbidities in COVID-19, clinicians will be able to revise their recommendations and management plans. Therefore it is important that we continue to share our experiences and outcomes during this pandemic.
References:
1. Cheng C-Y Lee Y-L Chen C-P et al., Lopinavir/ritonavir did not shorten the duration of SARS CoV-2 shedding in patients with mild pneumonia in Taiwan, J Microbiol Immunol Infect. 2020; published online April 3, DOI:10.1016/j.jmii.2020.03.032
2. Costanzo M De Giglio MAR Roviello GN , SARS-CoV-2: recent reports on antiviral therapies based on lopinavir/ritonavir, darunavir/umifenovir, hydroxychloroquine, remdesivir, favipiravir and other drugs for the treatment of the new coronavirus, Curr Med Chem. 2020; published online April 16, 2020, DOI:10.2174/0929867327666200416131117
3. WHO, 1 June 2020, Maintaining essential health services: operational guidance for the COVID-19 context, Website: https://www.who.int/publications/i/item/covid-19-operational-guidance-for-maintaining-essential-health-services-during-an-outbreak (Accessed 9/6/2020)
4. NHS Digital, Last updated 21 May 2020, Coronavirus (COVID-19): Shielded patients list, Accessed 29/5/2020, URL: https://digital.nhs.uk/coronavirus/shielded-patient-list
Loading Author...
Sign in or Register to comment