Coronavirus: NHS COVID-19 Deaths Analysed
The deaths of 119 NHS staff have been analysed by three leading clinicians and reported today in the HSJ. Thank you to Tim Cook, Emira Kursumovic and Simon Lennane for this report
The data they used are in the public domain. No attempts were made to contact families or other individuals to seek further information. Data were presented as summary data and no individuals are identified or identifiable. Analysis used simple proportions. Comparisons with national data are presented when relevant.
A case was considered fully confirmed when a minimum of three separate news outlets and one social media outlet had confirmed details. Where this was not possible the degree of verification was recorded. The name of the individual was preferred but not mandated. News and social media sites were checked regularly until the data set was closed at 1am on 22 April.
RESULTS
One hundred and nineteen cases were identified. Thirteen cases were excluded — in four cases multiple attempts to confirm information over several days were unsuccessful, in six cases the individual had retired and was not working, and in three the individual was not an active healthcare worker.
Among the 106 included cases, 98 had patient facing roles. In 89 cases they were able to establish the individual had been working during the pandemic. In no included cases was it clear they were not working, but there was no decisive evidence in 17.
The characteristics of the cases are presented in table 1. The date of death was known in 93% of cases and the rising number of deaths over time is shown in Figure 1, tracked against all UK deaths. For the last 10 days, healthcare worker deaths remain steady as a proportion of all UK deaths at 0.51-0.58 per cent.
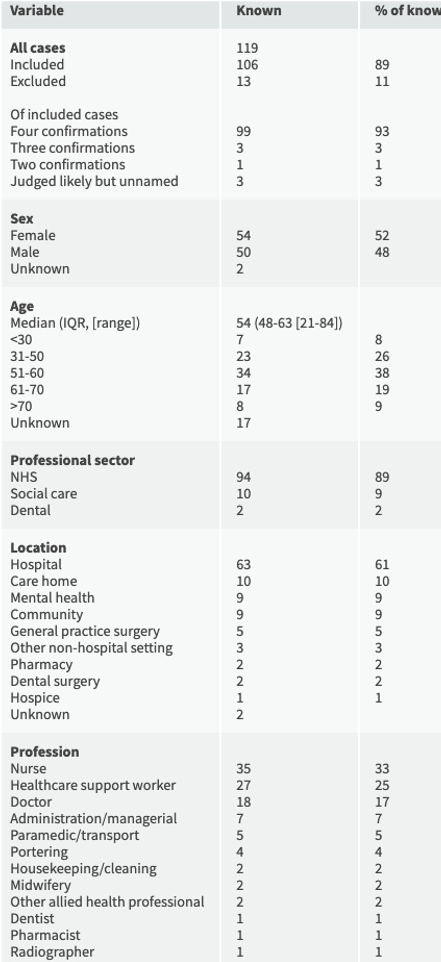
Among the doctors, the specialties involved were surgery (5), general practice (4), emergency medicine (2) and medicine (2), and one each from histopathology, geriatrics, neurorehabilitation, paediatrics, and psychiatry. There were no anaesthetists or intensivists identified.
Among the nursing staff, specialty was not always mentioned, but none were described as intensive care nurses. There were no deaths of physiotherapists reported.
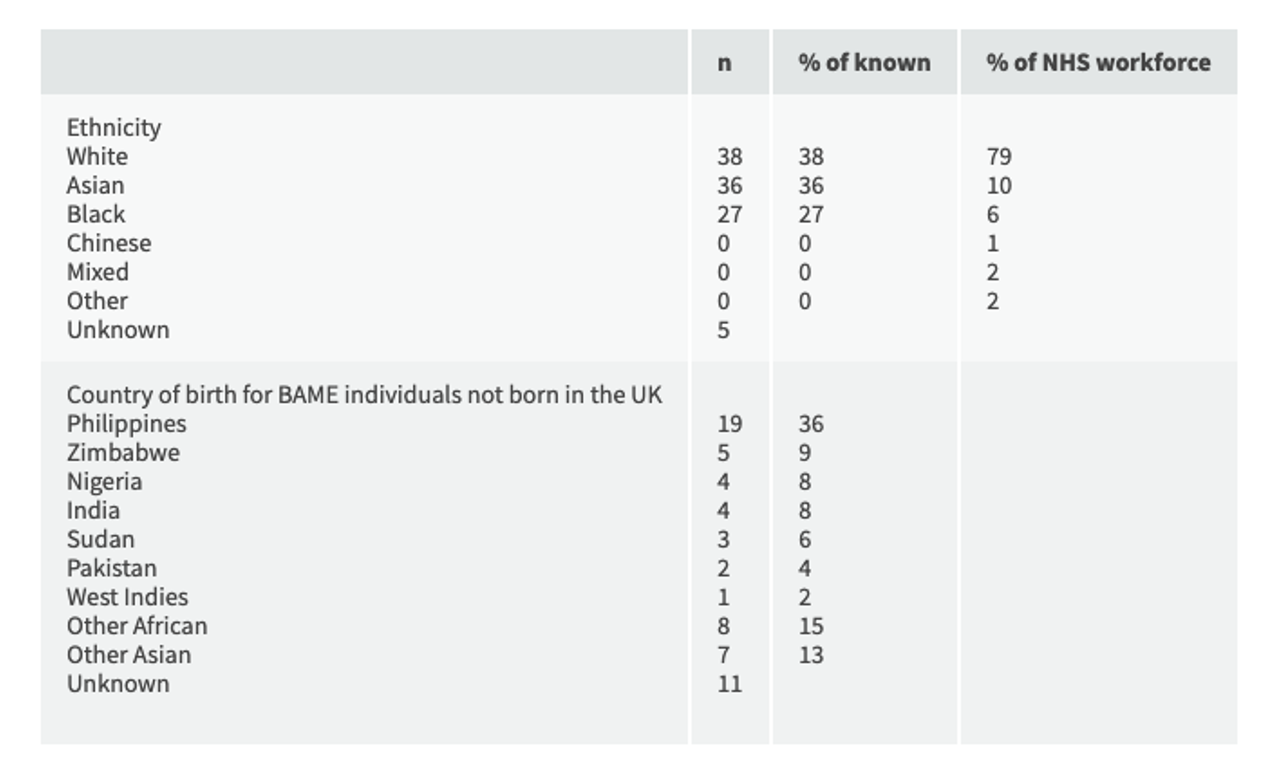
For 53 of 64 BAME individuals, their country of birth was not the UK and, for the other 11 (17%), this was uncertain. Among the Caucasian individuals, there were further staff who were not born in the UK, including three from elsewhere in Europe, meaning a minimum of 56 (53%) of those healthcare workers who died were not born in this country (Table 3).
COMMENTARY
There are three key findings from this analysis to highlight in particular:
· The disproportionately high rate of BAME individuals among those who have died;
· The absence of those members of staff considered at high risk of viral exposure and transmission; and
· The overall rate of fatalities compared to the population.
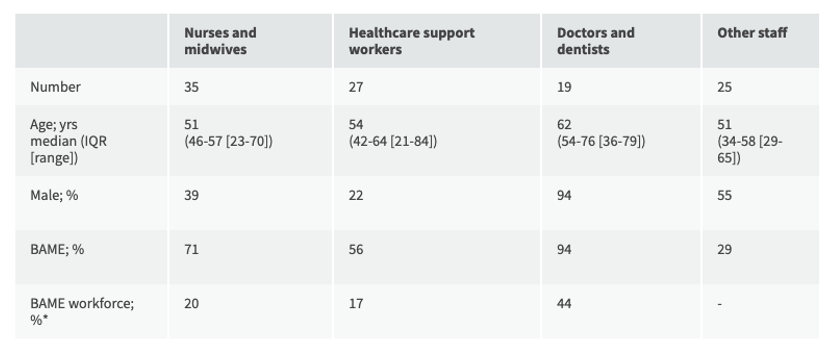
BAME account for 21% NHS staff - 20% nursing, and 44% medical staff
BAME account for 63% COVID19 NHS staff deaths - 64% of nursing, 94% of medical
BAME patients also accounting for 34% of the patients admitted to UK ITUs but only 17% of the population
The high number of deaths among Filipino staff has also been highlighted: with an estimated 40,000 such staff employed in the NHS they constitute a significant proportion of the nursing workforce.
There is a clear correlation between the cumulative UK deaths from Covid-19 in the UK population and among health and social care workers. The ratio is very close to 1:200 so the deaths among health and social care workers are approximately 0.5 per cent of all deaths, suggesting they are not overrepresented.
It is not possible to know whether infection occurred at home or at work, but they have determined that the vast majority of individuals who died had both patient-facing jobs and were actively working during the pandemic. It seems likely that, unfortunately, many of the episodes of infection will have occurred during the course of work.
The authors call for a central registry of deaths among health and social care workers to establish facts, enable robust rapid analysis and to explore whether social or employment inequalities are impacting on the rates of infection of these staff during the conduct of their duties and causing avoidable deaths.
There are immediate questions around precautionary actions to protect BAME NHS staff from harm and the duties that NHS Employers have in this regard.
The data include thankfully no staff who worked as nurses or doctors on ITU. The reasons are unclear but this is certainly the part of the healthcare system where PPE has been provided and used most comprehensively.
Loading Author...
Sign in or Register to comment