Chagas Disease - What You Need to Know

Chagas disease is a neglected tropical disease which is endemic in all continental Latin American countries. It is caused by trypanosoma cruzi, a parasite found in triatomine insects otherwise known as 'kissing bugs'. If left untreated, this parasitic infection can progress unnoticed over 10-30 years causing damage to the heart and gastrointestinal system. It is estimated that about 6 million to 7 million people worldwide are infected with the disease currently. Around 30% of patients infected with Chagas disease who are untreated will go on to develop cardiac dysfunction [1].
This video from the World Heart Federation provides an overview of Chagas disease and it's complications
This video references the World Heart Foundation IASC Roadmap on Chagas Disease 2021 which details a global call to action and practical solutions to tackling Chagas Disease worldwide.
What Can You Do to Fight Chagas Disease?
Control and Prevention
In Chagas endemic regions:
Spray houses and surrounding areas with insecticides to eliminate the bugs
Screen for Chagas disease in patients with non-specific symptoms (fever, fatigue, body aches, rash, headache, diarrhoea)
Screen all pregnant women and children of infected mothers
Screen blood and organ donors
Help build awareness of Chagas disease and it's complications to drive better detection and management of the disease
Treatment
Benznidazole or Nifurtimox is indicated for:
acute Chagas infection
those in whom the infection has been reactivated (for example, due to immunosuppression)
patients during the early chronic phase
Both medicines are nearly 100% effective in curing the disease if given soon after infection at the onset of the acute phase. The issue with these treatments is that they often cause side effects which can lead to non-adherence to the full 60 day course. The most common side effects (occurring in up to 40% of treated adults) are: a skin rash; weight loss; headache; and intense abdominal pain. The efficacy of both medications diminishes the longer a person has been infected and the adverse reactions are more frequent at older age.
If asymptomatic adults are diagnosed with Chagas disease through screening programmes, they should be offered treatment. This can prevent or slow disease progression towards the chronic gastrointestinal and cardiac complications.
Studies to investigate the optimum dose and treatment duration of these anti-parasitics are ongoing [2], this could lead to optimisation of care and help to reduce the burden of adverse effects driving non-completion of treatment.
Specific treatment for cardiac, digestive or neurological complications of Chagas disease may be required.
Chronic Chagas Cardiomyopathy
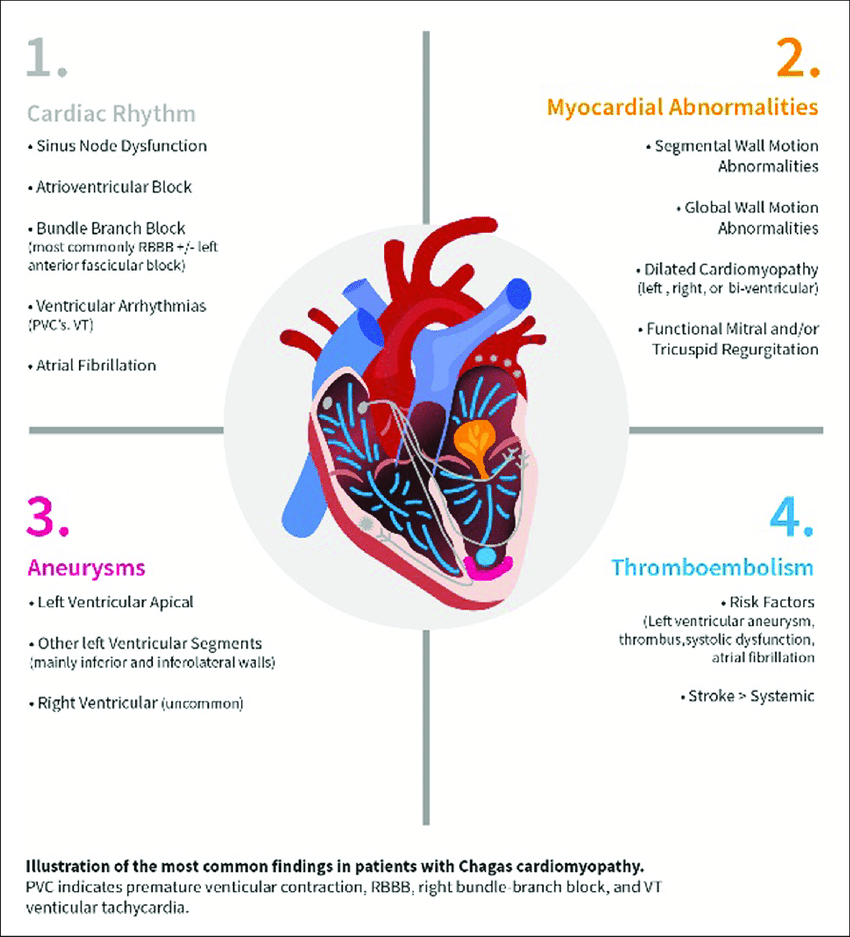
Illustration from WHF IASC roadmap on Chagas disease showing the most common findings in patients with Chagas disease [1].
Approximately 30% of patients with Chagas disease will go on to develop cardiac dysfunction. As can be seen in the image, this is due to prolonged scarring and inflammation. Importantly, Chagas disease patients have higher rates of conduction abnormalities, sudden cardiac death and thromboembolic events such as stroke than patients with cardiac dysfunction due to other causes [1]. It is therefore vital that chronic chagas cardiomyopathy (CCC) is treated with best medical therapy to improve patients quality of life.
As per globally accepted medical therapy for congestive heart failure, patients with CCC should be optimised where appropriate on:
beta-blockers
angiotensin-converting enzyme inhibitors/angiotensin receptor blockers
angiotensin receptor-neprilysin inhibitors (ARNI)
mineralocorticoid receptor blockers
Studies are ongoing to evaluate optimal medical therapy for CCC given it's unique physiology [1]
Management beyond medical therapies is often not available in low resources settings. However, implantable devices such as implantable cardioverter defibrillators (ICDs) and cardiac resynchronisation therapy (CRT) may be indicated as CCC progresses, and heart transplant surgery may also be indicated in certain circumstances.
We know that it can often be difficult to to detect or manage Chagas disease due to lack of resources in the rural areas in which it is endemic. At MedShr we are building a network of health care professionals interested in Chagas Disease to promote awareness and deliver education around the disease.
Join our Chagas Disease Global Education Network - through sharing your experiences of managing patients with Chagas Disease and your practical solutions to overcome barriers to detection and treatment, we believe this network will help to improve the lives of patients with Chagas Disease and ultimately save lives.


References
[1] Echeverría LE, Marcus R, Novick G, Sosa-Estani S, Ralston K, Zaidel EJ, Forsyth C, RIbeiro AL, Mendoza I, Falconi ML, Mitelman J. WHF IASC roadmap on Chagas disease. Global heart. 2020;15(1)
[2] Molina-Morant, D., et al. "Efficacy and safety assessment of different dosage of benznidazol for the treatment of Chagas disease in chronic phase in adults (MULTIBENZ study): study protocol for a multicenter randomized Phase II non-inferiority clinical trial." Trials 21.1 (2020): 1-10.
[3] WHO News Room - Chagas disease (also known as American trypanosomiasis): www.who.int/news-room/fact-sheets/detail/chagas-disease-(american-trypanosomiasis)
[4] Molina-Morant, D., et al. "Efficacy and safety assessment of different dosage of benznidazol for the treatment of Chagas disease in chronic phase in adults (MULTIBENZ study): study protocol for a multicenter randomized Phase II non-inferiority clinical trial." Trials 21.1 (2020): 1-10.
Loading Author...
Sign in or Register to comment