COVID-19 Investigation: Detecting Early Deterioration

How can we detect early deterioration in COVID-19, here are some resources and pathways that may be suitable for low and middle income countries (LMIC).
Epidemiological data has shown that majority of COVID-19 infections are mild, which means that with adequate assessment and triage majority of patients can be montitored at home or in the community. What tools are available for healthcare professionals in LMIC? Would any be suitable for general public use and education, to detect early deterioration in COVID-19?
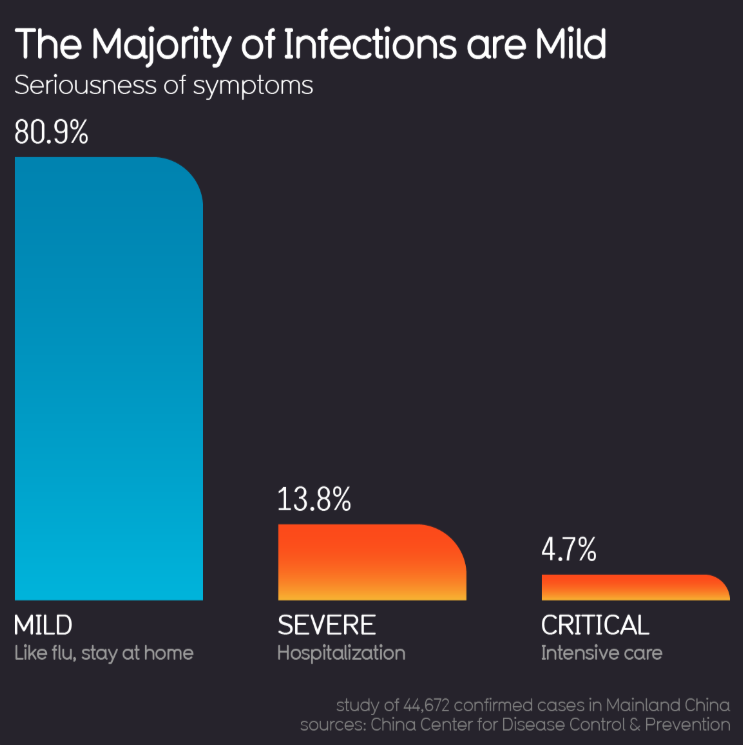
The COVID-19 death rates range from 1-7 % in literature, and in countries where only people requiring hospital admission are being screened (e.g. Italy and Spain), case fatality rates have exceeded 5%, which may be due to a smaller denominator in their analysis [1].
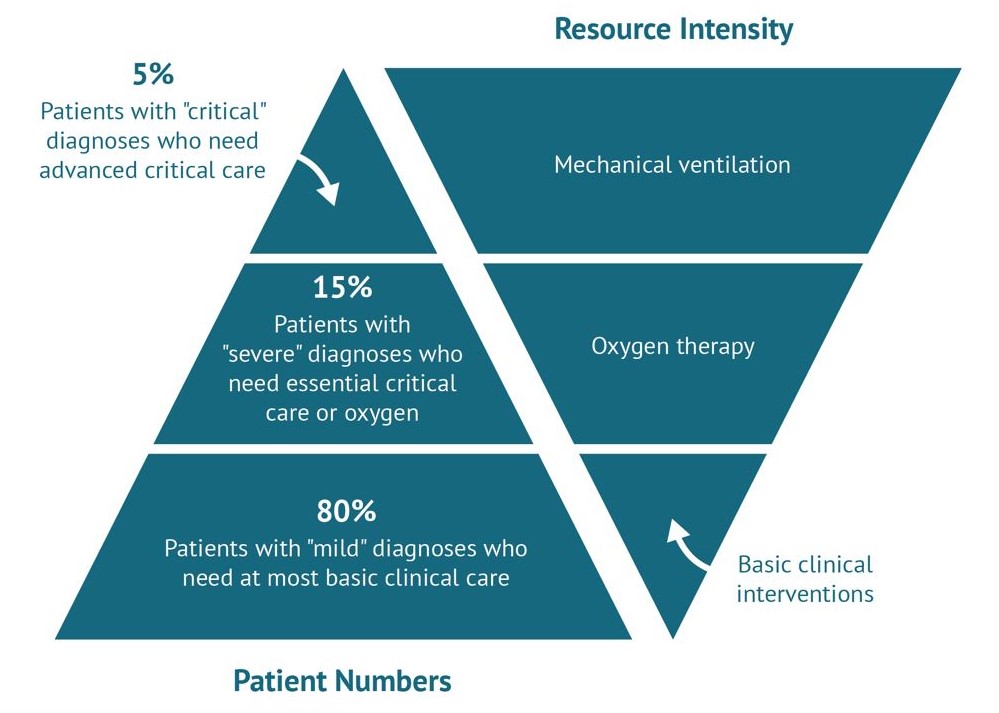
Unfortunately, though they form a minority of cases, the severe infections of COVID-19 will require more resources (e.g. medical equipment, medication, healthcare and support staff). Therefore detection of early deterioration and early intervention could help maximise resources and prevent deterioration.
Pathways of progression during COVID-19 infection - Can early intervention prevent adverse outcomes?
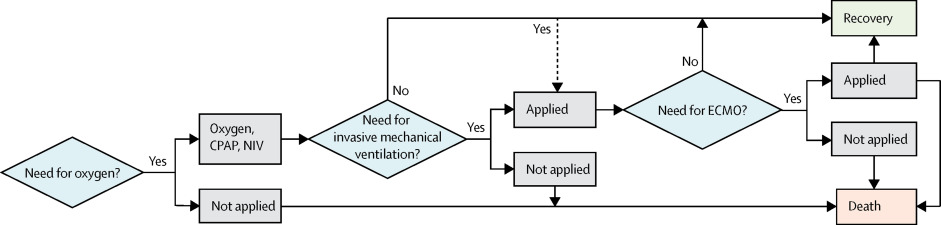
The real course of death from COVID-19 is thought to involve respiratory failure, but has also been attributed to shock and multi-organ failure, which makes the underlying cause less clear [1]. The precise role of secondary bacterial infection, co-infection and co-morbidities, such as tuberculosis, HIV and other infectious diseases are still unclear. The higher incidence of these communicable diseases may present more of a problem in LMIC during this pandemic, however data and outcomes from these patient groups are still emerging.
Example 1: The NEWS Score
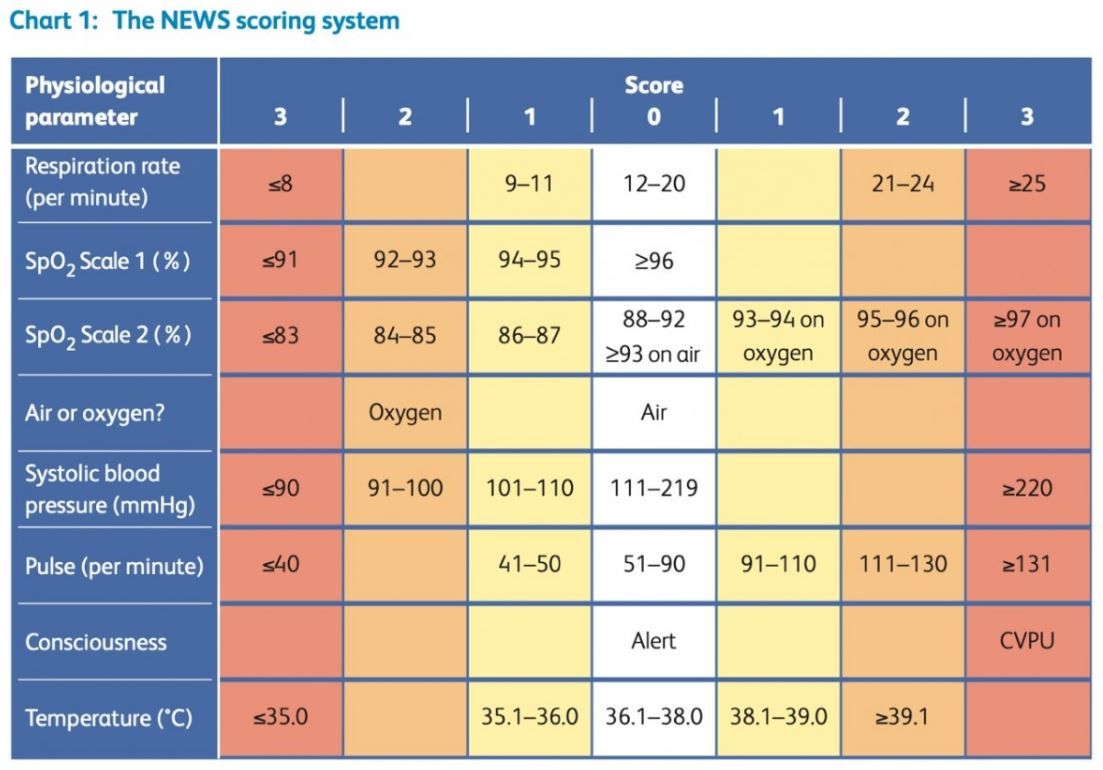
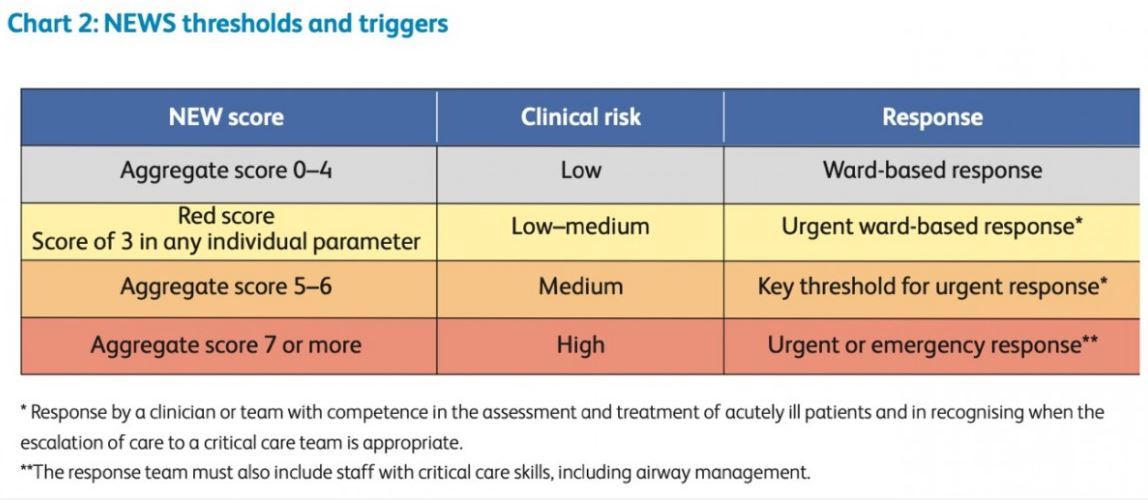
From the Royal College of Physicians (RCP), UK, the National Early Warning Score (NEWS) was launched in 2012 to improve the monitoring of patients in hospital [3]. This uses patient parameters (e.g. Heart rate, Respiratory rate, oxygen saturations, consciousness-level) to advise on the urgency of review/escalation.
An online NEWS Calculator can be found here, which includes an additional domain for the patient's suspected COVID-19 status.
Example 2: CXR Imaging Template
NHS England, the British Society of Thoracic Imaging and the Royal College of Radiologists, have created and endorsed a template for chest radiograph reporting for COVID-19 that can help reduce the burden of clinicians and radiographers and support the analysis and reporting during the pandemic. This may be more relevant for LMIC where performing serial radioiographs are more practical where high-resolution CT is limited. View the template here.
There is currently little evidence for early warning systems in COVID-19 [3]. Clinicians and healthcare professionals should therefore use their own clinical judgement and adapt existing protocols and guidance to the local situation. Escalating care in COVID-19 can be challenging in many LMIC where there is insufficient capacity in the secondary and tertiary healthcare units. Late presentation of infection may also make adapted early warning scores and protocols unreliable, therefore the examples featured here should serve as a guide and any decisions to adopt new guidelines or protocols should be agreed with your local/regional clinical governance teams.
References:
1. Vincent JL, Taccone FS. Understanding pathways to death in patients with COVID-19. Lancet Respir Med. 2020;8(5):430‐432. doi:10.1016/S2213-2600(20)30165-X
2. Ismail T, Baker T, Baker P, Chalidou K, Chi Y, Sullivan R, April 8, 2020, Strengthening the Basics: Approaches to COVID-19 Care in Low-Resource Settings, Centre for Global Development (Website), URL: https://www.cgdev.org/blog/strengthening-basics-approaches-covid-19-care-low-resource-settings (accessed 9.6.2020)
3. Centre for Evidence-Based Medicine, Nuffield Department of Primary Care Health Sciences, University of Oxford, April 2020, Website: NEWS (or NEWS2) score when assessing possible COVID-19 patients in primary care?, URl: https://www.cebm.net/covid-19/should-we-use-the-news-or-news2-score-when-assessing-patients-with-possible-covid-19-in-primary-care/ (Accessed 9/6/2020)
Loading Author...
Sign in or Register to comment